Alright guys, it’s time now to talk about the big V! When you hear about different birth control methods, whether through word-of-mouth, billboards, newspapers, TV or radio, you seldom hear anything about vasectomy. We want to talk to you about vasectomy now, explain away the myths and fears around it and shift the birth control discourse from the most common approach of what women should do to what men can do.
So what’s a vasectomy?
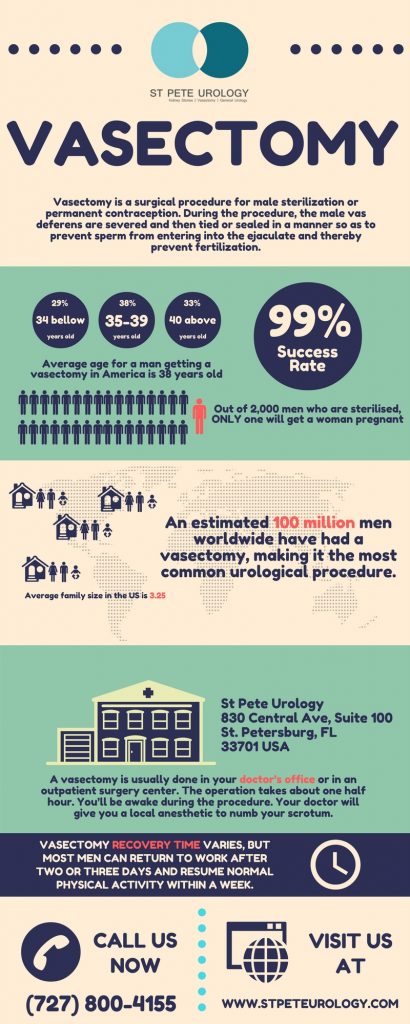
It is a simple, 15-minute non-drug permanent sterilization procedure for men. It’s performed under localized anesthesia and involves sealing off or cutting a portion of the sperm-conveying tubes (called vas deferens) in order to stop sperm from reaching the ovum when ejaculation occurs. If you are a man who has had all the children you wanted to have or are sure that you will never want to have any children in the future, vasectomy is a safe and cost-effective way to sterilize yourself.
Lots of questions
Yet, if you are like most men, you have probably heard the horror stories associated with vasectomy and you are worried that things may go wrong for you. Will it reduce my sexual pleasure? Will it turn me into a “eunuch” — a sad miserable man looking back constantly to his youthful years with nostalgia? And what if disaster strikes late in my life, or my life plans change, and I decide to have children? Can I reverse it? These and many more questions can make you have doubts about having a vasectomy. But it turns out these fears are baseless myths that shouldn’t stop you from a vasectomy.
What are the most frequent myths about vasectomy?
1. It will be intolerably painful
Honestly, for most men, the idea of the whole procedure can seem quite awkward. And since most of us have the habit of protecting our testicles from any type of direct assaults, a vasectomy seems like a real intrusion into a protected zone. But the truth is doctors who conduct vasectomies have gone through many years of study and training. They know what they are doing. They use the latest minimally invasive techniques to perform the procedure, ensuring that you feel no pain. The procedure is done under local anesthetic, so you will probably only have to worry about the needle going in. After that, you will remain aware of the procedure as it goes on but you will feel no pain or uncomfortable sensations.
2. Your penis won’t work
That’s wrong, mate. In reality, the procedure isn’t done anywhere near your penis — except of course if it’s causing an obstruction and the urologist has to move it out of the way. The snip is entirely about your balls and affects only those little tubes inside your balls that are called the vas deferens. Remember too that when you have sex and reach orgasm, the fluid that comes out, called ejaculate, is 97 percent semen and only 3 percent sperm. After vasectomy, you will still achieve orgasm and produce this ejaculate, except it won’t contain sperm and you won’t be able make your partner pregnant. That means your erections will remain exactly the same and your penis will stay as sensitive during sex as it was before the vasectomy. Likewise, your ability to enjoy sex and achieve orgasm will remain unchanged, though now you’ll be able to do so without having to worry about making anyone pregnant.
3. You will no longer ejaculate
That’s wrong, too. If you ejaculated before the snip, you’ll continue to do so after. Semen, the main component of ejaculatory fluid, is produced in the seminal vesicles and the prostate, which aren’t cut or blocked off during a vasectomy. And since only a small portion of fluid comes from the testicles with sperm, the overall volume of your ejaculate will reduce only slightly after a vasectomy — you won’t even notice it. Likewise, because the muscle contractions that propel fluid out during ejaculation typically come from the pelvis, your ejaculations won’t be affected by a vasectomy.
4. Your sperm production will shut down
Not true. Vasectomy doesn’t block sperm production and you’ll continue to make sperm after the snip. The only difference is that sperm will no longer reach semen and form part of the ejaculate. Because the sperm will go nowhere after a vasectomy, it will live for 3-5 days and decay naturally in the body. This is the same thing that happens naturally in men if they don’t ejaculate every 5 days or so. They produce sperm continuously but the sperm goes nowhere and is reabsorbed naturally in the body.
5. You can’t reverse it once it’s done
No, you can if you want. Vasectomy can be reversed through a surgical procedure called vasovasostomy (vasectomy reversal). During the procedure, the vas deferens (tubes) are reconnected, with each tube re-joined as it was before the snip in order to create a passageway for sperm, allowing sperm to again be present in semen. A successful reversal procedure restores your fertility and you can again make your partner pregnant. But when considering a vasectomy reversal, you need to consult an experienced urologist. That will ensure that no tissues are irreparably damaged during the reversal procedure.
6. Even if it’s reversed, you’ll remain impotent
Not really. With microsurgical advances currently used in vasectomy and vasovasostomy, the reversal has become more precise and more successful. So while vasectomy reversal is still technically expensive and demanding, doctors can now successfully restore a man to his pre-vasectomy condition. Although many men think that vasectomy can make them impotent, they should know that the procedure has no effect on blood flow to the spongy veins of the penis. These veins cause an erection. A vasectomy tends to make love-making more pleasurable and fun through the exhilarating feeling accompanying the ejaculation of spermless semen and also by erasing the fear of pregnancy.
7. It’s harder than a woman getting her tubes tied
A nice try indeed, but still wrong. Tubal ligation is performed under epidural or general anesthesia and typically takes longer than the 10-20 minutes required for a vasectomy. Tying a woman’s tubes also comes with a much more serious complication rate than a vasectomy. So why not just take the simpler route to contraception and block the source of sperm in order to remove the burden of birth control from women instead of looking for excuses to pressure women with contraception? After all, vasectomy is more effective than tubal ligation, costs much less and guarantees better results. In fact, for partners and couples considering family planning, vasectomy is a great cost-saving and effective solution to consider.
What if you are just one of those men who want to have multiple sexual partners without any additional responsibilities? Well, vasectomy works for that too. If you get a vasectomy, you can enjoy your lifestyle without having to worry about the possibility of fatherhood.
Want to know more about vasectomy? Speak with your partner and assess whether you have had all the children you want. Once you are sure of your decision, visit your doctor to discuss this birth control method. For more information on vasectomy and vasectomy reversal, visit the “St Pete Urology” site.




 Vasectomy is a more reliable method of preventing pregnancy than any other method of birth control. For instance, in comparison to the female equivalent called
Vasectomy is a more reliable method of preventing pregnancy than any other method of birth control. For instance, in comparison to the female equivalent called  Remember, a vasectomy means you will not be able to father a child, at least not without the huge cost and complications of reversal surgery. Therefore, you must never undertake vasectomy lightly. Before you and your partner choose this method of birth control, you should both consider it carefully. Talk to your
Remember, a vasectomy means you will not be able to father a child, at least not without the huge cost and complications of reversal surgery. Therefore, you must never undertake vasectomy lightly. Before you and your partner choose this method of birth control, you should both consider it carefully. Talk to your