 Erectile dysfunction (ED) is the inability to get or keep an erection that is strong enough for satisfactory sexual intercourse. That means even if you have no problem getting an erection, you could still have early stage erectile dysfunction if you are not able to achieve sexual satisfaction.
Erectile dysfunction (ED) is the inability to get or keep an erection that is strong enough for satisfactory sexual intercourse. That means even if you have no problem getting an erection, you could still have early stage erectile dysfunction if you are not able to achieve sexual satisfaction.
Early signs of erectile dysfunction
Occasional or intermittent sexual problems do not necessarily indicate erectile dysfunction. But you could have ED if the following are persistent:
- Reduced desire for sex
- Inability to get an erection
- Inability to maintain an erection
- Softer erections
- Lack of nighttime and early morning erections
Most men suffer from erectile problems at some point in their lives. When the symptoms are only occasional, it is not considered erectile dysfunction. But if they gradually and consistently gets worse, there is probably a physical cause—which is generally what happens in chronic erectile dysfunction. If the problem occurs suddenly, but the man can still have erections early in the morning and when masturbating, that suggests a mental cause, though something could be going on physically as well.
You should speak with a urologist about your sexual problems if:
Erectile dysfunction worries you enough to cause anxiety or threaten your relationship. The urologist will clear up the misinformation that could make your sexual problems worse and prescribe medication to help you through a rough patch.
- It is painful to get an erection or you find it difficult because your penis is curved (a condition called Peyronie’s disease).
- The problem is persistent and doesn’t go away. It could be a sign of a more serious underlying condition such as diabetes or coronary artery disease.
- Since causes of erectile dysfunction vary, and you may need a multi-teatment approach, seeing a urologist gives you the best chance of recovering quickly from the condition. Your doctor will help you determine the cause of your symptoms and then recommend treatment which may include lifestyle modifications, counseling, prescription medications (Viagra, Cialis, Levitra or Stendra), testosterone replacement, Alprostadil self-injection, Alprostadil urethral suppository, penis pump or penile implants.
At St Pete Urology, we understand that erectile dysfunction is frustrating and can have a profound impact on relationships and self-esteem. We also recognize that few men want to speak about their inability to get or maintain an erection. Each of our urologists is skilled, knowledgeable and experienced in helping men with this condition. We have a friendly and compassionate patient-centered approach that makes consultations confidential and beneficial. For more information about the treatment of erectile dysfunction and other urological problems, visit the St Pete Urology website.



 The testicles are the male reproductive organ. These oval-shaped organs are located in the scrotum just below the penis. The testicles have two primary functions: The first is to produce sperm and the second is to produce and discharge hormones, primarily testosterone. These two functions make them an indispensable part of the male reproductive system.
The testicles are the male reproductive organ. These oval-shaped organs are located in the scrotum just below the penis. The testicles have two primary functions: The first is to produce sperm and the second is to produce and discharge hormones, primarily testosterone. These two functions make them an indispensable part of the male reproductive system.
 Prostate health is an important part of overall health for men. The prostate is a walnut-sized gland situated between the bladder and the penis. The urethra, the tube through which urine exits the body, runs through the prostate. One of the prostate’s main functions is producing a fluid that nourishes and protects sperm. For men, the prostate is an important part of both the urinary and reproductive systems.
Prostate health is an important part of overall health for men. The prostate is a walnut-sized gland situated between the bladder and the penis. The urethra, the tube through which urine exits the body, runs through the prostate. One of the prostate’s main functions is producing a fluid that nourishes and protects sperm. For men, the prostate is an important part of both the urinary and reproductive systems.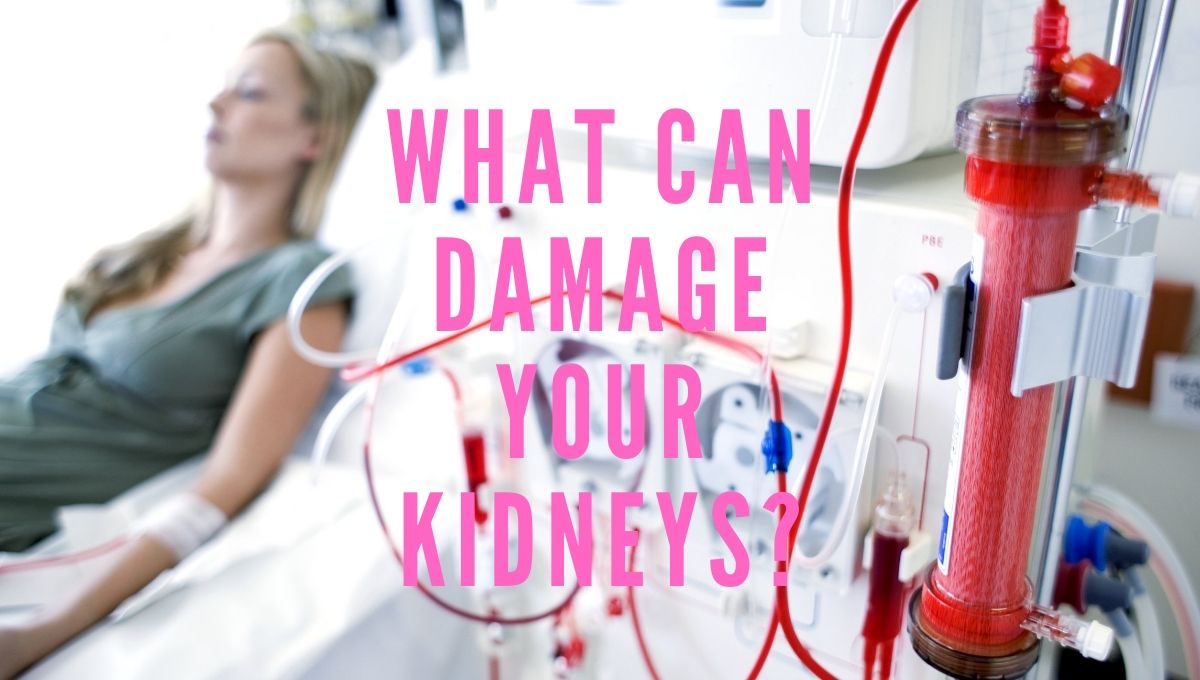
 The kidneys are a pair of organs located on either side of the spine just above the waist. Healthy kidneys work as your body’s filtration system. They help balance water and minerals in your blood. They remove waste from the blood that develops from digestion and muscle activity. In addition to filtration,
The kidneys are a pair of organs located on either side of the spine just above the waist. Healthy kidneys work as your body’s filtration system. They help balance water and minerals in your blood. They remove waste from the blood that develops from digestion and muscle activity. In addition to filtration, 
 The penis is one of the male body’s organs that is least likely to be harmed. Men are generally very careful not to damage their penises, but accidents do happen. The causes most often linked to penile trauma are car accidents, sport injuries, machine accidents, burns and gunshot wounds.
The penis is one of the male body’s organs that is least likely to be harmed. Men are generally very careful not to damage their penises, but accidents do happen. The causes most often linked to penile trauma are car accidents, sport injuries, machine accidents, burns and gunshot wounds.
 Reconstructive urology is a very important part of a patient’s urological treatment. For many different reasons, patients may find themselves in need of surgery to repair their urinary and reproductive systems. Everyone is different, so urologists assess each patient’s situation to determine the best treatment. A patient’s age, health and ability to recover from surgery are all factors a urologist will consider when determining if surgery is the best option.
Reconstructive urology is a very important part of a patient’s urological treatment. For many different reasons, patients may find themselves in need of surgery to repair their urinary and reproductive systems. Everyone is different, so urologists assess each patient’s situation to determine the best treatment. A patient’s age, health and ability to recover from surgery are all factors a urologist will consider when determining if surgery is the best option.
 There are many reasons why your primary care doctor may recommend a urologist. Urologists help patients with issues like
There are many reasons why your primary care doctor may recommend a urologist. Urologists help patients with issues like 
 Bladder problems are very common and can range from mild issues like a
Bladder problems are very common and can range from mild issues like a 
 A UTI, or urinary tract infection, is a painful but common condition. Approximately 50 percent of all women will experience a UTI in their lifetime, while 10 percent of men will deal with one. For many people, UTIs can become a recurring issue.
A UTI, or urinary tract infection, is a painful but common condition. Approximately 50 percent of all women will experience a UTI in their lifetime, while 10 percent of men will deal with one. For many people, UTIs can become a recurring issue. Because UTIs are normally
Because UTIs are normally 
 The prostate gland is an organ that is part of the
The prostate gland is an organ that is part of the