 If you are diagnosed with bladder cancer, there are several effective treatment options including chemotherapy, radiotherapy, and surgery. Your doctor will recommend the best treatment for you depending on your age, the stage of the cancer, the severity of the symptoms, and your overall health.
If you are diagnosed with bladder cancer, there are several effective treatment options including chemotherapy, radiotherapy, and surgery. Your doctor will recommend the best treatment for you depending on your age, the stage of the cancer, the severity of the symptoms, and your overall health.
At St Pete Urology, we use a shared decision-making approach in dealing with bladder cancer. Shared decision-making means that you and your urologist work together to arrive at a personalized treatment. We are very confident in the outcomes that we achieve through this approach.
So what is the most common treatment for bladder cancer?
Surgery is the most common treatment for bladder cancer. In fact, most people with the cancer need to undergo some form of surgery. And it is only because surgery may not remove all the tumor cells that the other treatments—chemotherapy, radiation, immunotherapy, targeted therapy—may be necessary along with or instead of surgery.
For early stage bladder cancer, the most common surgical procedure is transurethral resection of bladder tumor (TURBT), also called transurethral resection (TUR). During the procedure, the surgeon inserts a cystoscope through the urethra into your bladder and then uses a tool with a tiny wire loop, a laser, or high-energy electricity (fulguration) to remove the tumor.
If the bladder cancer is detected late, your surgeon may opt for cystectomy—a type of surgery that involves the removal of part of the bladder (partial cystectomy) or the whole bladder (radical cystectomy). Partial cystectomy is the ideal option for cancer that is still small and has spread only slightly to the muscle layer of the bladder.
But for cancer that is large or has spread deeper into the bladder muscle or to more than one part of the bladder, radical cystectomy is the go-to option. It is the removal of the whole bladder together with nearby tissues, organs and lymph nodes. In men, this may include the removal of the prostate gland, seminal vesicles, vas deferens, and part of the urethra. And in women, it can mean the removal of the uterus, ovaries, fallopian tubes, and part of the vagina.
Treatments used together with or instead of surgery
- Using medicines
Certain medications are effective in destroying cancer cells. Medications used to treat bladder cancer are usually in the form of chemotherapy, immunotherapy or targeted therapy.
- Chemotherapy
Chemotherapy is the use of drugs to destroy cancer cells. The drugs are administered in two ways: local (Intravesical) and whole-body (systemic).
For Intravesical chemotherapy, a prescribed drug is delivered to the bladder through a catheter inserted via the urethra. The drug destroys superficial tumor cells that come into contact with it, but may not be effective for deeper tumor cells or cancer cells that have spread to other organs. The most frequently used local therapy drugs are mitomycin-C, gemcitabine (Gemzar), docetaxel (Taxotere), and valrubicin (Valstar).
Systemic chemotherapy means that a drug or combination of drugs is taken orally or injected into the veins. The drug travels through the bloodstream to various parts of the body and shrinks, slows down or kills cancer cells that may have spread beyond the bladder.
Whole-body chemotherapy is done in cycles to give the body time to recover between treatments. Every cycle lasts a few weeks, while a complete treatment may take several months. Plus, systemic chemotherapy is often done before surgery to help shrink tumors, make them easier to remove, make surgery safer, and minimize the likelihood of a recurrence.
The drug cisplatin is the most commonly used systemic chemotherapy drug to treat bladder cancer, particularly for the most frequent type of the cancer, known as urothelial carcinoma. The drug damages the DNA of tumor cells so they can’t reproduce. Cisplatin is typically used in combination with other drugs. The most common combinations are:
- Methotrexate, vinblastine, doxorubicin (Adriamycin), and cisplatin (MVAC)
- Gemcitabine and cisplatin (GC)
iii. Cisplatin, methotrexate, and vinblastine (CMV)
- Paclitaxel, gemcitabine, and cisplatin (PGC)
- Dose-dense (DD)-MVAC, which has mostly replaced MVAC. It has the same regimen as MVAC, has a growth factor support, and administered with short time between treatments.
- Immunotherapy
The treatment exploits the body’s own immune system to attack cancer cells. The attack on cancer cells is triggered by materials made either by the body or in the laboratory. There are two types of immunotherapy: local and systemic.
In local immunotherapy, the doctor injects an immune-boosting germ, usually interferon or BCG (Bacillus Calmette-Guerin) into the bladder via a catheter. The material draws the body’s immune cells to the bladder and activates the cells to fight cancer cells.
Systemic immunotherapy is primarily focused on immune checkpoint inhibitors. The drugs used, such as Atezolizumab (Tecentriq), Avelumab (Bavencio), Nivolumab (Opdivo) or Pembrolizumab (Keytruda), have the ability to block the protein PD-1 found on the surface of T cells. Since protein PD-1 usually stops the immune system from destroying cancer cells, blocking it empowers the immune system to better eliminate cancer cells.
- Targeted therapy
The treatment involves using drugs that can target and destroy specific proteins, genes or tissues that enable the growth and survival of cancer cells. Drugs used, such as Erdafitinib (Balversa), Enfortumab vedotin—ejfv (Padcev) and Sacituzumab govitecan (Trodelvy), have the ability to block the growth and spread of cancer cells.
Before targeted treatment, the doctor runs genomic tests to identify the genes, proteins, and other factors contributing to the tumor. This helps to find the most specific molecular targets.
- Radiation therapy
It is the use of high-energy x-rays or other particles to destroy cancer cells. The treatment is administered in the form of external-beam radiation, which is radiation given from a machine located outside the body. The alternative, called brachytherapy or internal radiation therapy, which uses implants, is not ideal for bladder cancer.
A radiation therapy regimen, or schedule, consists of a specific number of treatments delivered over a set period of time.
For bladder cancer, radiotherapy is used:
- When you have early-stage bladder cancer
- When you have early-stage cancer but can’t have surgery
- As a follow-up to TURBT or partial bladder removal surgery
- To prevent or treat symptoms of advanced bladder cancer
Safe, unparalleled bladder cancer treatment
Are you experiencing bladder cancer symptoms? Or are you worried that your urinary symptoms could be due to bladder cancer?
At St Pete Urology, we have a team of urologists that are skilled, knowledgeable and experienced in bladder cancer diagnosis and treatment. So you can trust us to detect the cancer in its early stages and to administer the most appropriate treatment.
Through our collaborative, compassionate, multidisciplinary approach, we ensure that our patients get the best possible bladder cancer care. Visit us today for an accurate, timely diagnosis.
For more information on bladder cancer risks, prevention, signs and symptoms, diagnosis and treatment, visit the site “St Pete Urology.”



 Early diagnosis of bladder cancer is crucial for successful treatment. Unfortunately, there is no specific test available for screening asymptomatic people for the disease. So diagnosis of the cancer primarily relies on the presence of symptoms.
Early diagnosis of bladder cancer is crucial for successful treatment. Unfortunately, there is no specific test available for screening asymptomatic people for the disease. So diagnosis of the cancer primarily relies on the presence of symptoms. 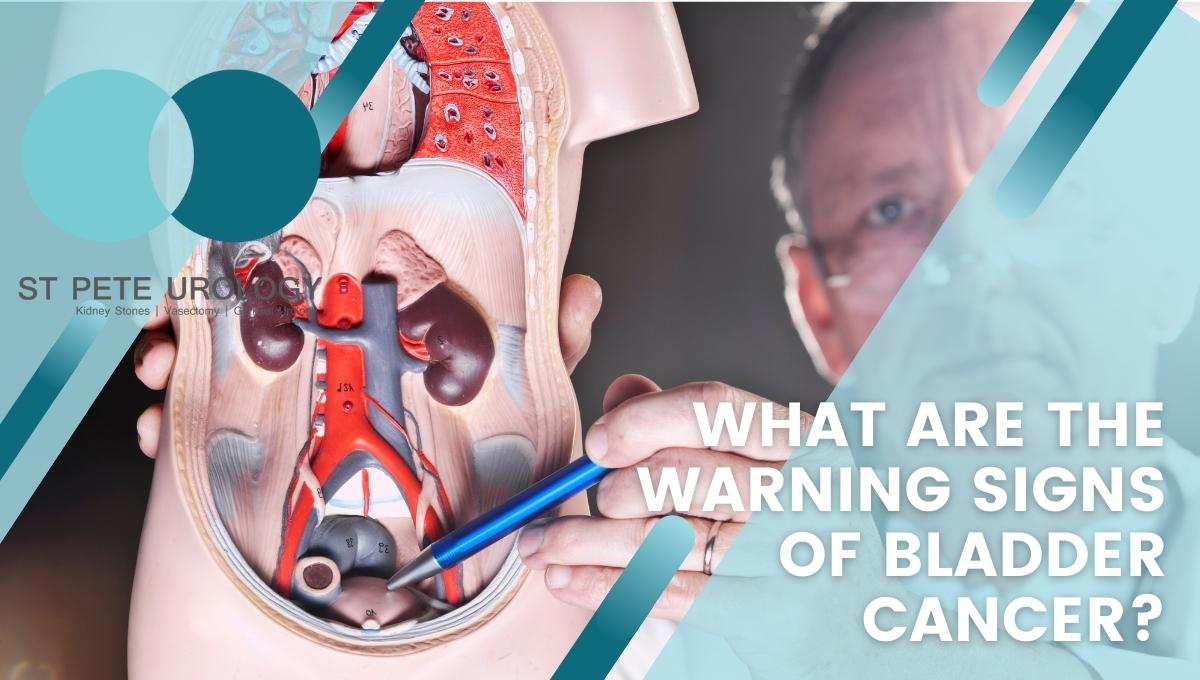
 Because the bladder holds urine produced by the kidneys, the warning signs of bladder cancer usually relate to urination. Urine is made in the kidneys and moves down the ureters to the bladder, which then stores the urine to allow for an infrequent, controlled urination.
Because the bladder holds urine produced by the kidneys, the warning signs of bladder cancer usually relate to urination. Urine is made in the kidneys and moves down the ureters to the bladder, which then stores the urine to allow for an infrequent, controlled urination.

 May is the World Bladder Cancer Awareness Month—a time to reflect on the burden of the cancer across the globe and to improve on the fight against the disease.
May is the World Bladder Cancer Awareness Month—a time to reflect on the burden of the cancer across the globe and to improve on the fight against the disease.
 Tonight we’re going to talk about bowel and bladder control primarily, so
Tonight we’re going to talk about bowel and bladder control primarily, so 
 With
With 
 You are experiencing some terrifying symptoms.
You are experiencing some terrifying symptoms.
 Urine is your body’s liquid waste. A larger part of it is water, but it also contains salts, urea, uric acid, and other chemicals. The contents of urine indicate how healthy your body is and an analysis of your urine sample can help your doctor to figure out if you’re healthy or not.
Urine is your body’s liquid waste. A larger part of it is water, but it also contains salts, urea, uric acid, and other chemicals. The contents of urine indicate how healthy your body is and an analysis of your urine sample can help your doctor to figure out if you’re healthy or not.